500+ Google Reviews
★★★★★ 4.9/5
4.9 out of 5
The best physios by far...
Truly outstanding experience...
...very friendly and welcoming.
...tons of experience.
...they have been amazing.
Hip pain can cause significant discomfort around the hip and groin, and can impact many activities of daily living including walking, stair climbing and running. Our expert Physiotherapists can help you get to the root cause of your hip pain and work with you to get back to full fitness.
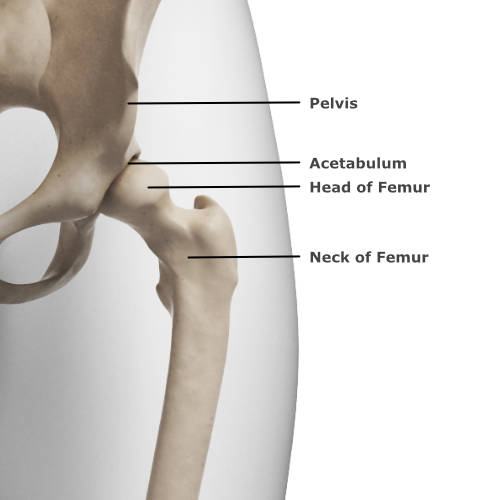
The hip joint is shaped like a ball and socket. The long thigh bone, the femur, has a ball shaped surface at the top where it sits into the socket of the pelvis. This socket is also called the acetabulum. It is the largest and deepest ball and socket joint in the body as it has the job of carrying your body weight. It fits very snugly whilst still allowing a lot of motion so we can walk, run, jump, squat and climb. There is cartilage between the ball and the socket called the labrum. This acts as a shock absorber.
Ligaments are tough fibrous structures that attach bones to each other. They act as stabilisers to prevent hypermobility in the a joint. The hip has several as it is a weight bearing joint and therefore needs very good stability.
There are lots of muscles around the hip. The best known are the Glutes. They are the power house and are found at the back of the hip, form the buttock and attach at the side of the hip joint. The Glutes allow you to stand up, stay upright, walk and climb stairs. The hamstrings are found at the back of the leg and attach to the pelvis on the sitting bones. The ITB or iliotibial band goes down the side of the leg and attaches below the knee and helps stabilise the hip. The Quads or quadriceps are the large muscles down the front of the leg. They attached from the front of the pelvis to the knee. The hip flexor (Iliopsoas) is another large contributor to hip strength and stability. It originates on the lumbar spine and attaches to the top of the femur.
Nerves around the hip include the sciatic nerve at the back, and the femoral nerve at the front. There is also a small nerve called the obturator nerve.
Hip osteoarthritis is a joint disease which causes gradual damage to the cartilage in the hip joint, eventually damaging the articular surfaces of the joint itself. It is the second most commonly affected joint after the knee and around 2.5 million people in England are affected.
People who suffer with hip osteoarthritis most commonly present with pain in the groin area. They also have pain and stiffness with certain movements of the hip joint – usually when trying to bring the knee towards the chest, take the leg out to the side or when rotating the leg inwards. They may also have difficulty with usual daily activities like walking, bending down to tie their shoelaces, climbing stairs and getting in and out of a chair or car.
Hip osteoarthritis can be diagnosed using an X-ray, however it is common that the amount of changes shown on the X-ray do not correlate with the persons’ clinical symptoms. For example, there are people who have very severe changes on x-ray but in the absence of pain and vice-versa.
Risk factors for hip osteoarthritis include age, sex (women twice as likely as men), genetics, history of joint dysplasia or joint laxity, and high body mass index. Excessive exercise involving repeated heavy loading or impact, as well as heavy manual labour may also advance the condition. Most cases tend to have a combination of the above.
Physiotherapy for hip osteoarthritis aims to reduce the stress on the joint by giving advice on activity-modification and strengthening the surrounding muscles. Manual techniques may be employed to help ease the joint stiffness and improve mobility. There are many people who manage their symptoms well with Physiotherapy and a long-term exercise programme.
For those with more severe pain or disability, injections into the hip joint may help ease some of the symptoms when done in collaboration with a Physiotherapy programme. Total hip replacement is known to be a successful surgical option for treating osteoarthritis.
Greater trochanteric pain syndrome (GTPS) or Lateral Hip Pain are the terms used to describe pain on the lateral side of the hip. The condition was previously referred to as Trochanteric Bursiitis; due to advances in research however, it appears inflammation of the bursa plays a much smaller part in the condition than previously thought.
GTPS is thought to result from compressive or tensile over-load of the structures at the lateral aspect of the hip. Symptoms include pain over the lateral aspect of the hip which can sometimes radiate down the lateral aspect of the thigh and into the buttock. These symptoms can be exacerbated or triggered by side lying, crossing one’s legs, sitting in low chairs and walking or running.
GTPS generally responds well to conservative treatment; 90% of cases resolve with physiotherapy, relative rest and in some cases cortisone injections. The aims of physiotherapy treatment are to reduce or alter load on the painful structures in the short-term while improving the load tolerance through a specific, graded exercise programme.
The hamstrings are a group of three muscles at the back of the thigh. They originate from the ischial tuberosity of the pelvis (the sitting bone) and run down the back of the leg to the knee.
Hamstring injuries are common in the athletic population. High hamstring tendinopathy is a particularly common injury among distance runners. The condition usually presents as a well localised pain in the top part of the thigh or buttock. It is often exacerbated by running, squatting, lunging and sitting (particularly on hard surfaces). Walking up-hill or up-stairs can also be painful.
High hamstring tendinopathy is thought to occur due to compression of the hamstring tendon where it attaches to the pelvis, under load. This can occur due to increased speed-work, hill-work or increased mileage without adequate preparation. Other factors including age, sex, weight and lifestyle may also contribute to the symptoms.
The initial treatment of high hamstring tendinopathy aims to reduce pain. This will likely mean reduced running or no running for one to three weeks. Rehabilitation will focus on progressive glute and hamstring strength and conditioning in positions of minimal pain. As the pain settles your physiotherapist will advise you on a graded return to running and an exercise programme to continue to optimise glute and hamstring recruitment and control.
The lower limb connects to the trunk through the hip joint, which is a ball and socket joint. The socket in which the ball fits is made deeper by a rim of cartilage known as the labrum.
FAI (Femoroacetabular Impingement), is a condition where the contact between the ball (known as the femoral head) and the socket (called the acetabulum) becomes painful. FAI is common in both males and females and can be due to irregularities in the bony shape of either the ball or socket of the hip.
An x-ray can be helpful in diagnosing the condition. Day to day movements where the leg is raised, such as walking, running and stair climbing can aggravate FAI and it is usually felt around the hip or groin region. Sports such as football (which include lots of twisting, running and change of direction) can also aggravate and contribute to FAI. Other symptoms of stiffness and a sensation of catching in the hip may occur. Imbalances in surrounding hip muscles can contribute to FAI as well.
Many patients recover from FAI through a specific Physiotherapy rehabilitation programme. Initially, avoiding the painful movements and activities is important, and gradually working on strengthening the hip can allow one to get back to high level exercise. For some, further interventions including injections and surgery may be necessary.
A hip labral tear involves the ring of cartilage between the ball and socket of the hip joint. Tears can occur traumatically during contact sports such as Football (lots of twisting and turning), but also in Ballet dancers and Yoga where the hip can move to extreme range of movement. Tears can also occur gradually over time, through wear of the hip joint and especially if there are structural irregularities in the hip joint such a FAI (Femeroacetabular Impingement).
Symptoms include a locking, catching or clicking felt deep in the hip joint. Pain from a labral tear is usually located in the hip and groin region, and the hip may feel stiff with reduction to range of movement. X-ray and MRI scans are used to diagnose a labral tear.
First line treatment usually involves Physiotherapy and hip injection, to help settle the pain symptoms and work on increasing the strength and range of movement in the hip joint. If this fails to manage symptoms, surgery may be indicated to repair the tear.
A thorough examination comprised of specific questions and physical tests can help to diagnose the cause of your hip pain. A treatment plan would then be discussed and implemented, to help you towards being pain free and get you back to performing your desired activities. A fundamental part of the treatment plan is explaining the cause of pain and ways to manage it.
Treatment could include hands-on therapy (joint mobilisation/soft tissue massage), a programme of stretches or strength based exercises, Taping, Acupuncture, Ultrasound or perhaps Shockwave Therapy (if appropriate).
If further investigations such as MRI, Ultrasound scan, blood tests or X-rays are required, our Physiotherapists can point you in the right direction. If the Physiotherapist feels you need to see another health professional (such as an Orthopaedic Consultant or Rheumatologist), they will ensure you see the right person via our vast network and close links with consultants.
So, if you have been struggling recently with hip pain, click here to contact us so we can help you get better!
We usually call you back within the hour during normal working hours
We usually respond within the hour during normal working hours